First aid training: why every workplace underestimates it

First aid training is often treated as a basic requirement rather than as a serious operational control. That mindset misses what happens in the first minutes after an injury, collapse, burn, cut, chemical splash, or crush event. Before external responders fully take over, coworkers and supervisors may be the only people able to stabilize the situation, control the scene, and pass accurate information forward.
Many organizations underinvest because they assume real emergencies are rare, the training expires into theory, or one designated first aider is enough for the whole site. In practice, response quality depends on coverage, confidence, role clarity, and how well people can act under stress. A strong first aid training program does more than teach technique. It shapes how a workplace behaves during the most chaotic opening moments of an incident.
Why the first minutes matter more than many teams admit
The period between injury and professional medical handover is often messy. Equipment may still be running, access may be poor, witnesses may panic, and nobody may know immediately who should call emergency services, who should guide responders, and who should keep the area from getting worse. Training helps convert that confusion into a usable sequence of actions.
The benefit is not limited to life-threatening events. Even moderate injuries are handled better when people know how to assess urgency, protect themselves, gather information, and avoid worsening the condition through well-meaning but unsafe improvisation. Response quality also affects later reporting and investigation because the first trained observers are often the ones who notice the earliest facts.
This is why first aid training should be viewed as part of emergency readiness, not as a standalone class. It works best when it is linked to alarms, site access, communication flow, and the likely injury scenarios created by the site's own tasks and materials.
What a practical first aid training program should include
A useful program combines core medical response principles with site-specific scenarios. Participants should know how to assess the scene, protect themselves, call for help, and support the injured person until handover. Just as important, they should understand the boundaries of their competence so they do not create new harm while trying to help.
Practical drills matter because stress changes behavior. People who understood the theory in a classroom may still freeze when the alarm sounds, blood is visible, or several people start speaking at once. Short scenario-based practice is what turns abstract knowledge into usable action.
The program should also define coverage. One trained person per site is rarely enough if shifts, remote areas, vehicle work, contractors, or after-hours activity are involved. Coverage planning determines whether the training can actually reach the scene in time.

Where many workplaces get the program wrong
A common mistake is assuming certificate status equals readiness. Attendance records show who completed the course, but they do not prove that the right people are present on the right shifts or that the team can coordinate under pressure. A second mistake is failing to align training with the site's real injury profile. Office scenarios will not prepare a maintenance crew, and a generic class may not suit a chemical handling area.
Another weakness appears when equipment and training drift apart. First aid supplies, eyewash points, stretchers, access routes, or emergency contacts may change over time while the course content stays frozen. The workforce then remembers one version of the response while the physical environment now requires another.
Sites also underestimate the supervisory role. Supervisors may not deliver treatment, but they often control access, communication, crowd management, and the handoff to responders. If they are excluded from the training logic, the response can fragment quickly.
How to keep skills usable between formal courses
Refresher learning should be shorter and more frequent than many companies expect. Mini drills, scenario talk-throughs, equipment checks, and quick response walkthroughs help teams remember what matters without turning every month into a full certification exercise. These moments also reveal where assumptions have changed since the last formal class.
It helps to vary the scenarios. Heat stress, falls, cuts, eye exposure, vehicle incidents, and lone-worker events all stress the response differently. Repeating only one familiar exercise may keep confidence high while leaving major blind spots untouched.
The best refreshers are linked to actual site change. New layouts, contractor activity, staffing changes, new materials, and lessons from recent incidents should all influence what the team practices next.
Where first aid training fits in the wider response system
The course is only one part of readiness. Equipment placement, communication flow, access control, incident reporting, and emergency coordination all affect whether trained people can act effectively when a real event occurs. A site that trains well but leaves kits empty, routes blocked, or roles unclear will still struggle under pressure.
This is why leadership should review first aid readiness together with drills and incident lessons. The question is not simply whether the certificate is current. The question is whether the site can deliver timely, coordinated support in its actual operating conditions.
When organizations want stronger practical response, Safety On can help align first aid training with coverage, site layout, likely scenarios, and the wider emergency system people depend on when seconds matter.
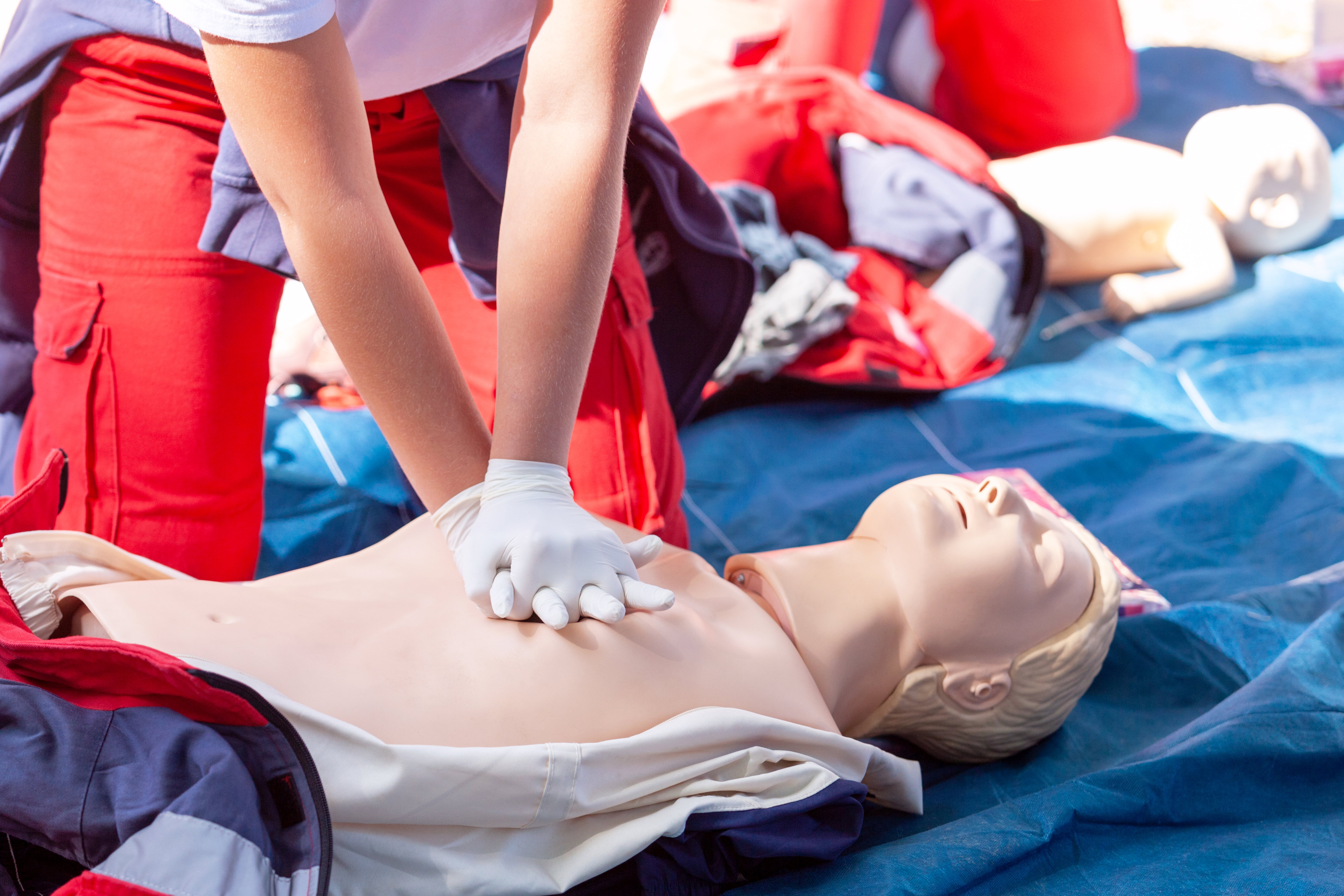
Coverage, equipment, and scene control after the class ends
Training only works if the site can support it operationally. First aid kits, eyewash stations, stretchers, route access, emergency contact lists, and scene-control expectations all have to match what people learned. If the class teaches one response flow while the site layout forces another, confidence disappears quickly during a real event.
Coverage planning matters just as much as content. A workplace may have several trained people overall and still be weak on nights, weekends, remote corners, or contractor-heavy periods. Reviewing who is available by shift and area often reveals response gaps that certificate counts alone never show.
The response also needs coordination rules. One person may focus on the injured worker, another on emergency services, another on access control, and another on initial reporting. When those responsibilities are discussed in advance, the first aid training becomes much more useful because people know where their role begins and ends.
Equipment checks should be folded into this routine. A missing item, blocked kit, or outdated contact list can undermine good training very quickly because the responder now has knowledge without the tools or information needed to act on it.
Even a short site walk after refresher training can uncover those mismatches. It reminds the team that emergency response depends on placement, access, and communication just as much as on medical technique.
FAQ
How often should first aid training be refreshed?
Formal renewal depends on local requirements and the provider model, but practical refreshers should happen more often. Changes in staffing, layout, scenarios, and incident lessons are strong reasons to revisit the response before the next certificate date.
Who needs this emergency response training in a workplace?
At minimum, the site needs enough trained people to cover all relevant shifts and work areas. Supervisors and roles that coordinate response also benefit because they influence access, communication, and emergency handover. Remote and lone-work situations deserve special attention too.